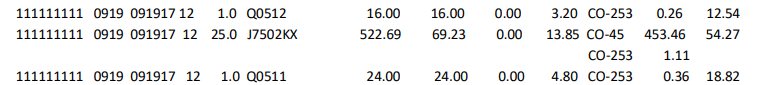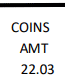Remittance Advice Instructions Tool
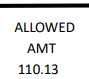
Hover over the image of Standard Paper Remittance Advice (SPR) to view information and descriptions. Many of the descriptions will also apply to the Electronic Remittance Advice (ERA), though they may not appear in the same order.