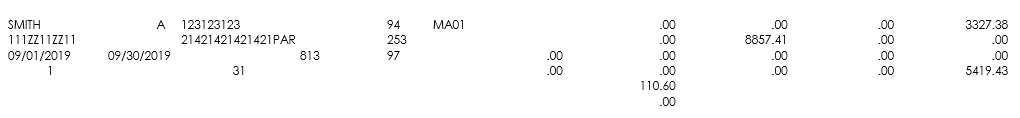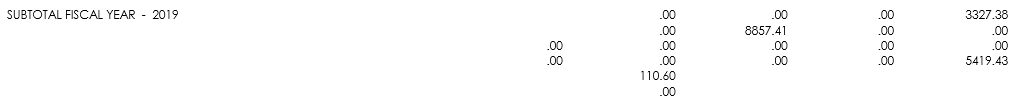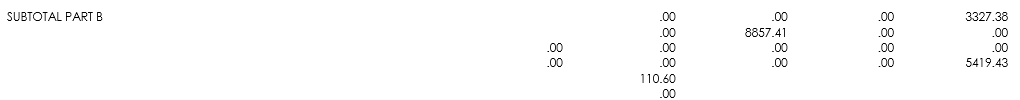Interactive Medicare Standard Paper Remittance (SPR) Advice
Interactive Medicare Standard Paper Remittance (SPR) Advice
The Medicare Remittance Advice (RA) is a notice sent to home health and hospice providers explaining how billing transactions are processed (paid, rejected, or denied). Billing transactions include final claims, adjustments, and canceled, denied, or rejected claims as well as Requests for Anticipated Payments (RAPs). SPRs are not provided if the HH&H has received the Electronic Remittance Advice (ERA) for more than 30 days. However, providers who have registered for myCGS (the CGS Web portal) are able to view and print standard paper remittances.
This interactive guide provides an overview of the SPR Advice. Select the section (below) that you wish to view. As you move your mouse over the area of interest, the field(s) will highlight and the name of the field will display. Click on the field to view more detailed information.
The SPR includes two sections:
- All Claims (AC) page(s) show information for each individual claim (not the individual charges on the claim). Claims will be listed on separate pages depending on whether the services apply to Medicare Part A or Part B.
- Summary page includes information that encompasses all the claims included in the AC section.
All Claims (AC) Page
The All Claims (AC) page includes information for each individual claim (not the individual charges on the claim). Claims will be listed on separate pages depending on whether the services apply to Medicare Part A or Part B.
As you move your mouse over the area of interest, the field(s) will highlight and the name of the field will display. Click on the field to view more detailed information.
Summary Page
The Summary page includes information that encompasses all the claims included in the AC section.
As you move your mouse over the area of interest, the field(s) will highlight and the name of the field will display. Click on the field to view more detailed information.
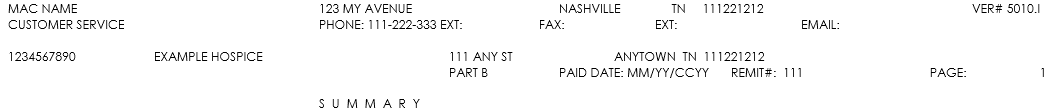
Medicare Administrative Contractor (MAC) and Provider Information |
||
The CLAIM DATA section of the summary page displays totals for all the billing transactions references on this SPR. |
This section of the summary page contains Pass through amounts. These fields do not apply to home health and hospice billing transactions. |
|
Not functional. |
This section of the summary page displays all provider payments made on this SPR and can be used for transaction-level balancing. To obtain the total payment amount (NET PROVIDER PAYMENT), add all the amounts in the PAYMENTS section. Then subtract the amount shown in the TOTAL WITHHOLD field, which is a negative amount representing the total of all provider adjustments. |
|
Heading for the COST, COVDY and NCOVDY information. |
Not functional |
|
Summary of the total number of days applied to the Medicare Cost Report (MCR) for billing transactions processed on this SPR. Not applicable to home health and hospice billing transactions. |
An additional payment made to a hospital for services provided by an intern or resident physician. Not applicable to home health and hospice billing transactions. |
Heading for the payment recap section of the summary page. |
Summary of covered home health or hospice days or visits for billing transactions processed on this SPR. |
An additional payment amount made to a certified hospital for a kidney acquisition. Not applicable to home health and hospice billing transactions. |
The total DRG outlier amount for billing transactions processed on this SPR. Not applicable to home health and hospice billing transactions. |
Summary of non-covered home health or hospice days for billing transactions processed on this SPR. |
The dollar amount of reimbursable bad debts. These debts include coinsurance and deductibles that a hospital is unable to collect from a beneficiary. Not applicable to home health and hospice billing transactions. |
The total amount of interest paid by Medicare for billing transactions processed on this SPR. Interest is paid on clean billing transactions if Medicare payment is not made within 30 calendar days. Reference: Medicare Claims Processing Manual, Pub. 100-04, Ch. 1, Section 80.2.2 |
The reimbursement amount a hospital receives for Certified Registered Nurse Anesthetist (CRNA) services. Not applicable to home health and hospice billing transactions. |
The total procedure code payable amounts for billing transactions processed on this SPR. Not applicable to home health and hospice billing transactions. |
|
Heading for the COVD, NCOVD and DENIED information. |
A total of the pass thru amounts in the Pass Thru Amounts section of the SPR. Not applicable to home health and hospice billing transactions. |
The total net reimbursement amount made to the provider for billing transactions processed on this SPR. |
Summary of covered charges for billing transactions processed on this SPR. |
A total of the pass thru amounts in the Pass Thru Amounts section of the SPR. Not applicable to home health and hospice billing transactions. |
|
Summary of non-covered charges for billing transactions processed on this SPR. |
The dollar amount of the Periodic Interim Payment (PIP) paid to the provider. Not applicable to home health billing transactions. |
The dollar amount of the Periodic Interim Payment (PIP) paid to the provider. Not applicable to home health billing transactions. |
Summary of denied charges for billing transactions processed on this SPR. |
The refund amount issued for settlement payments. |
The refund amount issued for settlement payments. |
The dollar amount of an accelerated payment made to a provider. |
||
Indicates refunds unrelated to settlement payments. |
Indicates refunds unrelated to settlement payments. |
|
Summary of the professional component amount for billing transactions processed on this SPR. |
The dollar amount of money being released previously withheld from a provider on penalty withhold. |
The dollar amount of money being released previously withheld from a provider on penalty withhold. |
Summary of MSP payment made for billing transactions processed on this SPR. |
The amount of a Transitional Outpatient Payment. Not applicable to home health and hospice billing transactions. |
The total TOP amount paid on this SPR. Not applicable to home health and hospice billing transactions. |
Summary of deductible payments owed to the provider by beneficiaries for billing transactions processed on this SPR. |
An additional payment amount an inpatient hospital receives for the hemophilia blood-clotting factor. Not applicable to home health and hospice billing transactions. |
The total hemophilia add-on amount paid on this SPR. Not applicable to home health and hospice billing transactions. |
Summary of the coinsurance amount owed to the provider by beneficiaries for billing transactions processed on this SPR. |
An additional dollar amount Medicare paid for 'new technology' drugs and devices. Not applicable to home health and hospice billing transactions. |
The total dollar amount of funds Medicare paid for 'new technology' drugs and devices on this SPR. Not applicable to home health and hospice billing transactions. |
This field represents the amount associated with value code 'Q7' (ISLET Add-On Payment Amount). |
This field represents the amount associated with value code 'Q7' (ISLET Add-On Payment Amount). |
|
The amount of a check/payment that has been voided and reissued. Not applicable to home health and hospice billing transactions. |
The total amount of a check/payment that has been voided and reissued on this SPR. |
|
Not applicable for home health and hospice services |
Not applicable for home health and hospice services |
|
The outstanding balance owed to Medicare that is carried forward to the next SPR. For additional information, refer to the "Remittance Advice (RA)/Electronic Remittance Advice (ERA) Payment Summary Page and Forward Balances (FB)" article on the CGS website. |
||
Summary of the beneficiary refund amount for billing transactions processed on this SPR. |
This section of the summary page includes the amount(s) withheld from payments. |
The total amount withheld for billing transactions processed on this SPR. This amount is the sum from the WITHHOLD FROM PAYMENTS section of the SPR. |
Summary of the interest paid to the provider for clean billing transactions that were not processed within the 30-day timeframe. |
The amount withheld from the current SPR's net reimbursement and applied to an existing claim receivable balance. The claim receivable balance would have been created and carried forward from a net negative reimbursement on a previous SPR. A net negative reimbursement is usually caused by a cancellation or adjustment to a previous paid billing transaction. When the net negative reimbursement exceeds total payments, a claim receivable balance carries forward and offsets future payments. CGS recommends that you monitor negative net reimbursement totals on SPRs in order to identify the claim receivable withholdings that are recouped on future SPRs. |
This amount displays when forced balancing of the SPR is required. |
Summary of the contractual adjustment amount for billing transactions processed on this SPR. |
The dollar amount being withheld to recover an accelerated payment previously paid to the provider. |
The net amount being paid to the provider. This amount should match the check amount issued to the provider. |
Summary of the procedure code payable amount for billing transactions processed on this SPR. |
The payment amount withheld from a provider due to an unfiled Medicare Cost Report, a payment suspension or a credit balance report not being submitted in a timely manner. |
|
The total dollar amount that a provider receives for billing transactions included on this remittance advice. |
The dollar amount withheld from a provider due to an unpaid settlement owed to Medicare. |
The check or Electronic Funds Transfer (EFT) transaction number through which payment was issued. |
The dollar amount withheld from a provider due to a third party payment. |
||
The payment amount withheld from an affiliated provider. |
||
The payment amount withheld from a provider due to a recoupment owed to Medicare. |
||
The payment amount withheld from a provider due to overdue taxes owed to the Internal Revenue Service (IRS). |
||
The payment amount withheld from a provider due to unpaid debts. Typically, these withholdings are Treasury requested offsets for unpaid Medicare or VA overpayments of the provider or an affiliated providers. |
||
A total of the withholding amounts in the Withhold From Payments section of the SPR. |
||
Updated: 11.16.20