J15 HHH Postpayment Resumptive Review Status Update 08/17/2020—12/31/2020
Beginning August 17, 2020, CMS directed the MACs to resume fee-for-service medical review activities beginning with postpayment reviews of items/services provided before March 1, 2020. Items and services are selected based upon high error rates and/or potential overutilization identified through data analysis.
CGS Medical Review is dedicated to the integrity of the Medicare program. CGS welcomes provider inquiries and continues to offer education sessions to ensure providers understand CMS regulations with the goal of successful reviews resulting in claim payment.
Results for service specific postpayment reviews are listed below.
5L000 Home Health Medical Necessity |
|
|---|---|
Reviews Completed |
532 |
Claims Allowed |
288 |
Claims Denied |
244 |
No Provider Response |
53 |
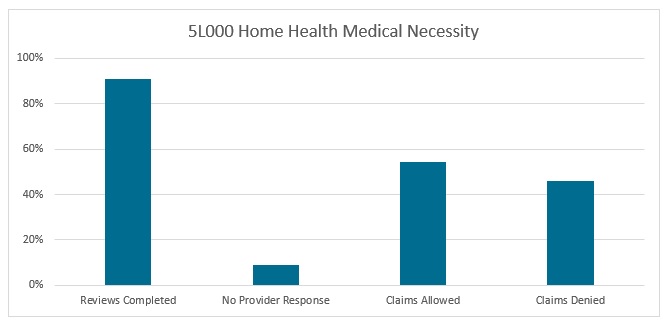
Top Finding: 5HC01 The physician certification was invalid since the required face-to-face encounter was missing/incomplete/untimely. Refer to CMS Medicare Benefit Policy Manual (Pub. 100-02, Ch. 7![]() ), CGS Home Health Face-to-Face (FTF) Encounter Web page and Home Health Denial Fact Sheet: Missing/Incomplete/Untimely Face-to-Face Encounter
), CGS Home Health Face-to-Face (FTF) Encounter Web page and Home Health Denial Fact Sheet: Missing/Incomplete/Untimely Face-to-Face Encounter![]() and Face-to-Face (FTF) Encounters for Home Health Certification
and Face-to-Face (FTF) Encounters for Home Health Certification![]() Quick Resource Tools.
Quick Resource Tools.
Resources:
- CMS Medicare Benefit Policy Manual (Pub. 100-02, Ch. 7
 )
) - CGS Educational Materials and Resources Web page
- CGS Home Health Top Medical Review Denial Reason Codes Web page
5M000 Hospice LOS > 730 Days |
|
|---|---|
Reviews Completed |
80 |
Claims Allowed |
39 |
Claims Denied |
41 |
No Provider Response |
5 |
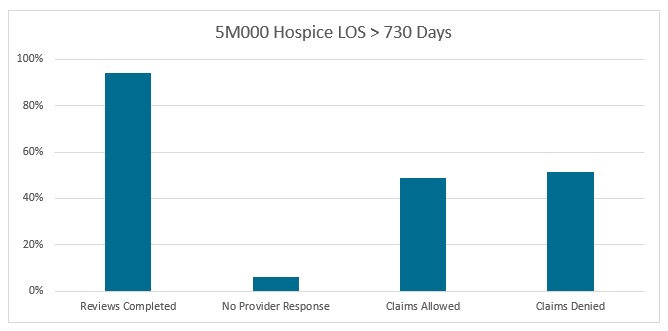
Top Finding: 5PM01 According to Medicare hospice requirements, the information provided does not support terminal prognosis of six months or less. Refer to CMS Medicare Benefit Policy Manual (Pub. 100-02, Ch. 9![]() ), Hospice Local Coverage Determination (LCD), “Determining Terminal Status”
), Hospice Local Coverage Determination (LCD), “Determining Terminal Status”![]() , and CGS Hospice Denial Fact Sheet—Six-Month Terminal Prognosis Not Supported
, and CGS Hospice Denial Fact Sheet—Six-Month Terminal Prognosis Not Supported![]() , Suggestions for Improved Documentation to Support Medicare Hospice Services
, Suggestions for Improved Documentation to Support Medicare Hospice Services![]() , and Appropriate Clinical Factors to Consider During Recertification of Medicare Hospice Patients
, and Appropriate Clinical Factors to Consider During Recertification of Medicare Hospice Patients![]() Quick Resource Tools.
Quick Resource Tools.
5M001 Hospice GIP ≥ 7 days |
|
|---|---|
Reviews Completed |
51 |
Claims Allowed |
17 |
Claims Denied |
34 |
No Provider Response |
5 |
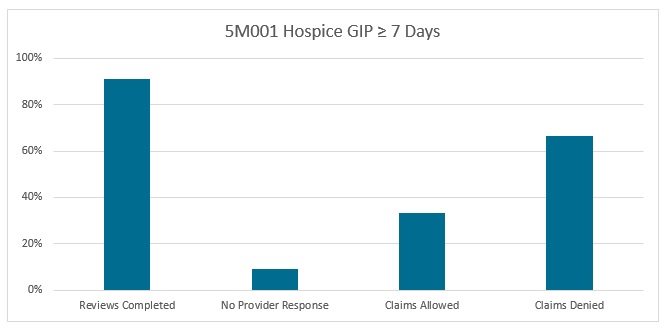
Top Finding: 5PM02 According to Medicare hospice requirements, the documentation indicates the general inpatient level of care was not reasonable and necessary. Therefore, payment will be adjusted to the routine home care rate. Refer to CMS Medicare Benefit Policy Manual (Pub. 100-02, Ch. 9![]() ) and CGS General Inpatient Care Web page and Hospice Denial Fact Sheet/Denial Reason 5PM02: Reduced Level of Care (Medical Necessity), Denial Reason 5PX03: Reduced Level of Care (Technical)
) and CGS General Inpatient Care Web page and Hospice Denial Fact Sheet/Denial Reason 5PM02: Reduced Level of Care (Medical Necessity), Denial Reason 5PX03: Reduced Level of Care (Technical)![]() Quick Resource Tool.
Quick Resource Tool.
Resources:
- CMS Medicare Benefit Policy Manual (Pub. 100-02, Ch. 9
 )
) - CGS Educational Materials and Resources Web page
- CGS Hospice Top Medical Review Denial Reason Codes
- CGS Medical Review Additional Development Request (ADR) Process Postpayment Review Web page
Provider inquiries and education requests may be emailed to J15HHMREDUCATION@cgsadmin.com.
CGS encourages providers to request education and conduct self-monitoring based on our posted Medical Review activity log and by using tools such as Comparative Billing Reports (CBRs) offered through our web portal.
To learn more about the postpayment resumptive process, please refer to the following links:

